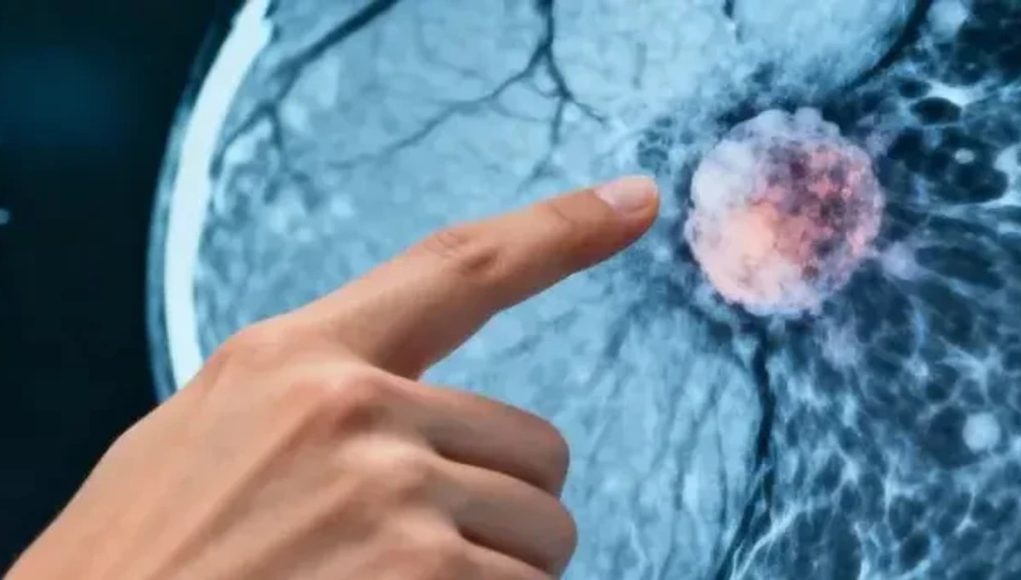
The presence or absence of malignant cells at this key point helps doctors choose the next steps of treatment
Do you know what the sentinel lymph node is, the so-called “guard”? It is the first lymph node where cells from the tumor area arrive and which can be the first to indicate whether the disease is spreading. For this reason, its analysis plays an important role in making decisions about further treatment.
How do lymph nodes participate in the spread of disease
Lymph nodes are small but very important organs of the lymphatic system, distributed throughout the body and connected to the network of lymphatic vessels. Lymph, a clear fluid that removes excess fluid, metabolic waste, and immune system cells, especially lymphocytes, from tissues, constantly circulates through them.
The role of lymph nodes is not only “passive filtration”. They actively participate in the immune response, recognizing and stopping bacteria, viruses, but also damaged or altered cells. Precisely because of this function, they represent one of the first places where tumor cells that have broken away from the primary tumor can stop.
In a large number of malignant diseases, the spread does not immediately go to distant organs, but first affects the lymph nodes near the tumor. Therefore, their status has important diagnostic and prognostic value.
Sentinel lymph node – first in line
The sentinel lymph node is defined as the first node to which lymph from the tumor area arrives, i.e. the place where there is the greatest possibility that the first metastatic cells will appear.
It is important to note that the sentinel node is not “determined” in advance, its position depends on the anatomical path of the lymphatic drainage of the relevant organ or region. In breast cancer, these are most often the nodes in the armpit, while in melanoma they are found in the lymphatic basin closest to the site of the change in the skin. In certain cases, there may be several sentinel nodes, reports Buz Post.
What is a sentinel lymph node biopsy and why is it done?
A sentinel lymph node biopsy is a standard diagnostic procedure used to assess whether the disease has spread beyond the primary tumor.
The procedure involves identifying this “first” node, surgically removing it, and analyzing it for pathology. The finding has a direct impact on determining the stage of the disease and the subsequent treatment plan.
A negative result means that there are no tumor cells in that node and that the likelihood of spread to other lymph nodes is low. A positive result indicates the presence of metastases and a higher risk of further spread, which requires additional evaluation and often a different therapeutic approach.
How to find the “sentinel” node
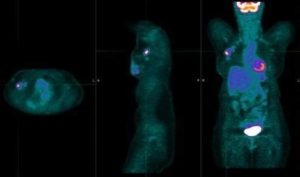
To locate the sentinel node precisely, a radioactive tracer, special dye, or a combination of the two is injected near the tumor. These substances follow the natural flow of lymph and “mark” the first node it reaches.
The surgeon then, using a probe or by sight, identifies that node and removes it through a small incision. The procedure is most often performed at the same time as the surgery to remove the tumor, but it can also be done separately, depending on the clinical situation.
Advantages over classic lymph node dissection
Previously, in some cancers, a larger number of lymph nodes were routinely removed from a given region, which increased the risk of complications.
Sentinel node biopsy allows for a much more selective approach. If the result is negative, the patient can avoid extensive surgery and its consequences, without compromising the accuracy of the disease assessment.
This approach today represents the standard in breast cancer and melanoma, where numerous studies have shown that it does not negatively affect survival, while significantly reducing unwanted effects.
Possible complications and limitations
Although it is a less invasive procedure, sentinel node biopsy carries certain risks. The most important of these is lymphedema, swelling that occurs due to impaired lymph flow, especially if a larger number of nodes are removed.
Pain, numbness, infection, or lymph fluid collection at the surgical site may also occur. There is also the possibility of a false-negative result, when the sentinel node does not contain tumor cells, even though they have already spread further.
For this reason, the results are always interpreted in the context of the entire clinical picture./BuzPost/